Coding
CMS Failure to Rescue quality measure financial impact hitting soon
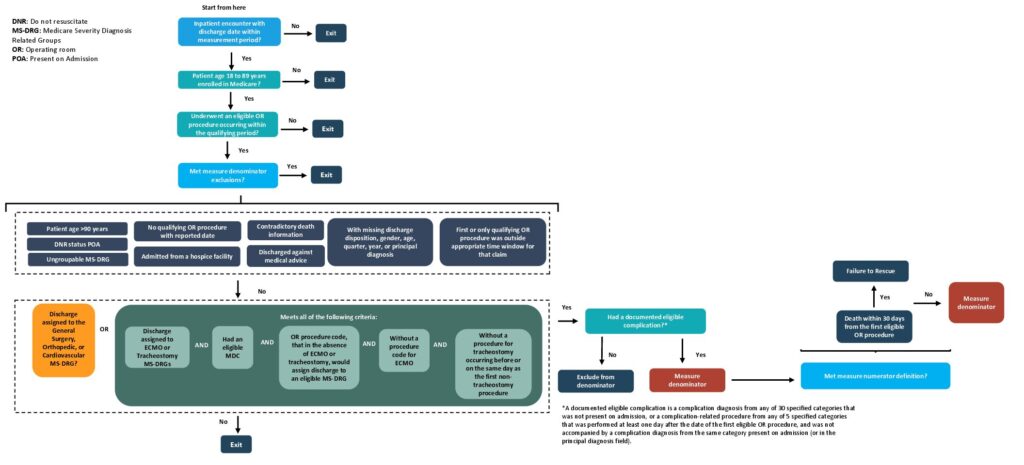
By Brian Murphy A reminder: The new CMS Failure to Rescue (FTR) quality measure is going to hit hospital pocketbooks—possibly your own—on October 1. Key details of the new CMS FTR measure (FY 2025 IPPS Update) Definition: The percentage of surgical inpatients who experience a complication and subsequently die within 30 days of their initial…
Read MoreIf a GLP-1 drops your BMI under 35, is morbid obesity off the table?
By Brian Murphy At the ACDIS conference last week, an interesting obesity coding question posed during a Q&A session at the Outpatient Symposium: Should we continue to code morbid obesity for patients who were previously morbidly obese (BMI greater than 35 with obesity-related comorbidities), but because they are on an active GLP-1 their BMI is…
Read MoreA must watch: New CMS video signals new metric for Medicare Advantage
By Jason Jobes The 2027 Medicare Advantage final rate notice is out—and the buzz is everywhere. Let me just say I rarely pause to watch a video, much less one that is 20 minutes. This one is a MUST watch if you are in risk adjustment. Last week “Health Tech Nerds” hosted an interview with…
Read MoreGrassley Report of UnitedHealth Group takes aim at these 20 diagnoses: Here’s why
By Brian Murphy The Grassley Report examining the risk adjustment practices of UnitedHealth Group (UHG) is much more than just a one-time media splash. The report is 105 pages long and contains a wealth of information and insight into how UHG does its work. This includes the criteria it uses to report diagnoses to…
Read MoreMedicare Advantage plans: Should healthcare organizations care about payer audits, fines? Hint: Yes
You are a CDI Director at a large integrated healthcare system, with oversight of staff working in acute care hospitals and clinics. You have patients with Aetna and Kaiser Permanente. Then the news hits: Kaiser agrees to pay $556M to settle false claims act (FCA) allegations for inflated risk adjustment coding. Aetna, $117M for similar…
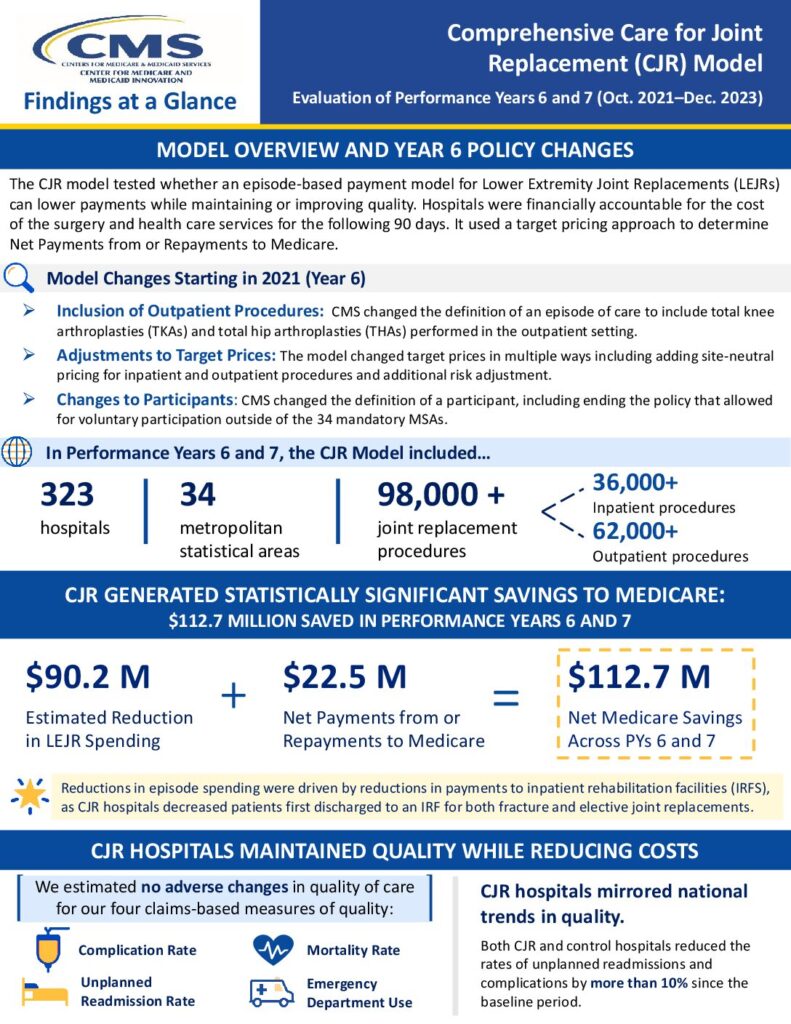
Read MoreFinancial success of Comprehensive Care for Joint Replacement (CJR) model paved way for TEAM
By Brian Murphy The Comprehensive Care for Joint Replacement (CJR) model is over, and it generated savings to Medicare. How much? We await the grand total, as final performance year financial results are expected later this year. But the latest, just released data (see attached graphic) shows that the CJR generated a whopping $112.7…
Read MoreNew Norwood special report examines latest trends in payer denials
Download the report here. Denials are being turned up, not down. But they’re happening in less noticeable and more insidious ways, often under a different name. Aided by new AI technologies, payers are finding increasingly creative ways to deny claims outright or blanket reduce payments–a soft equivalent to a denial. This report examines some of…
Read MoreYou need to have it both ways: Audits must target missed coding opportunities and invalid conditions in risk adjustment
By Brian Murphy Among the alleged behaviors that led to Kaiser’s eventual $556M payout to settle false claims act allegations was its aggressive effort to only add diagnosis codes (up to a year or more after the encounter) and never remove them. This is called a one-way audit, and the Department of Justice does not…
Read MoreFive things to know about Present on Admission (POA) for hospital payment, quality
By Brian Murphy Present on admission (herein POA) for coding purposes is defined as conditions that are present at the time the order for the inpatient admission occurs. It’s important to get POA status right, as it impacts payment and quality metrics. POA conditions (as reported with a Y) count as CCs or MCCs, whereas…
Read MoreHow a baseline became a springboard to documentation, coding improvement
What gets measured, gets managed. An old business truth … but we don’t always think of the inverse. Without a baseline, you won’t know where to focus. An integrated healthcare system comprised of county-owned hospitals and clinics suspected it was leaving severity and revenue on the table, but wisely didn’t want to dive straight into education without a clear starting line. With its provider and coding teams busy delivering care and getting claims out the door it turned to Norwood for help. Our work …
Read More