CMS Failure to Rescue quality measure financial impact hitting soon
By Brian Murphy
A reminder: The new CMS Failure to Rescue (FTR) quality measure is going to hit hospital pocketbooks—possibly your own—on October 1.
Key details of the new CMS FTR measure (FY 2025 IPPS Update)
- Definition: The percentage of surgical inpatients who experience a complication and subsequently die within 30 days of their initial operating room procedure.
- Scope: Focuses on patients 18+ admitted for general surgery, orthopedic, or cardiovascular MS-DRGs.
- Reporting Period: Commenced with the July 1, 2023 – June 30, 2025 reporting period, impacting FY 2027 payments.
- Data Source: Claims data.
- Purpose: Replaces PSI-4 (Death Rate Among Surgical Inpatients with Serious Treatable Complications) to focus specifically on the probability of death given a postoperative complication.
The FY 2027 payment period starts Oct. 1, 2026. Hospitals that fail to meet reporting requirements lose 25% of their annual IPPS market basket update. A big hit.
Claims-based measures like FTR usually require no data submission, but from what I could find a hospital could fail to meet reporting requirements by not submitting required electronic quality measures for two quarters, or failing chart-abstracted validation requirements. And you want to perform well, because it is used on sites that report hospital quality to the public.
Good CDI and inpatient coding work can impact your performance in the measure. FTR performance is derived from ICD-10 codes, risk adjusted, and active on a rolling basis for FY 2028 and subsequent years.
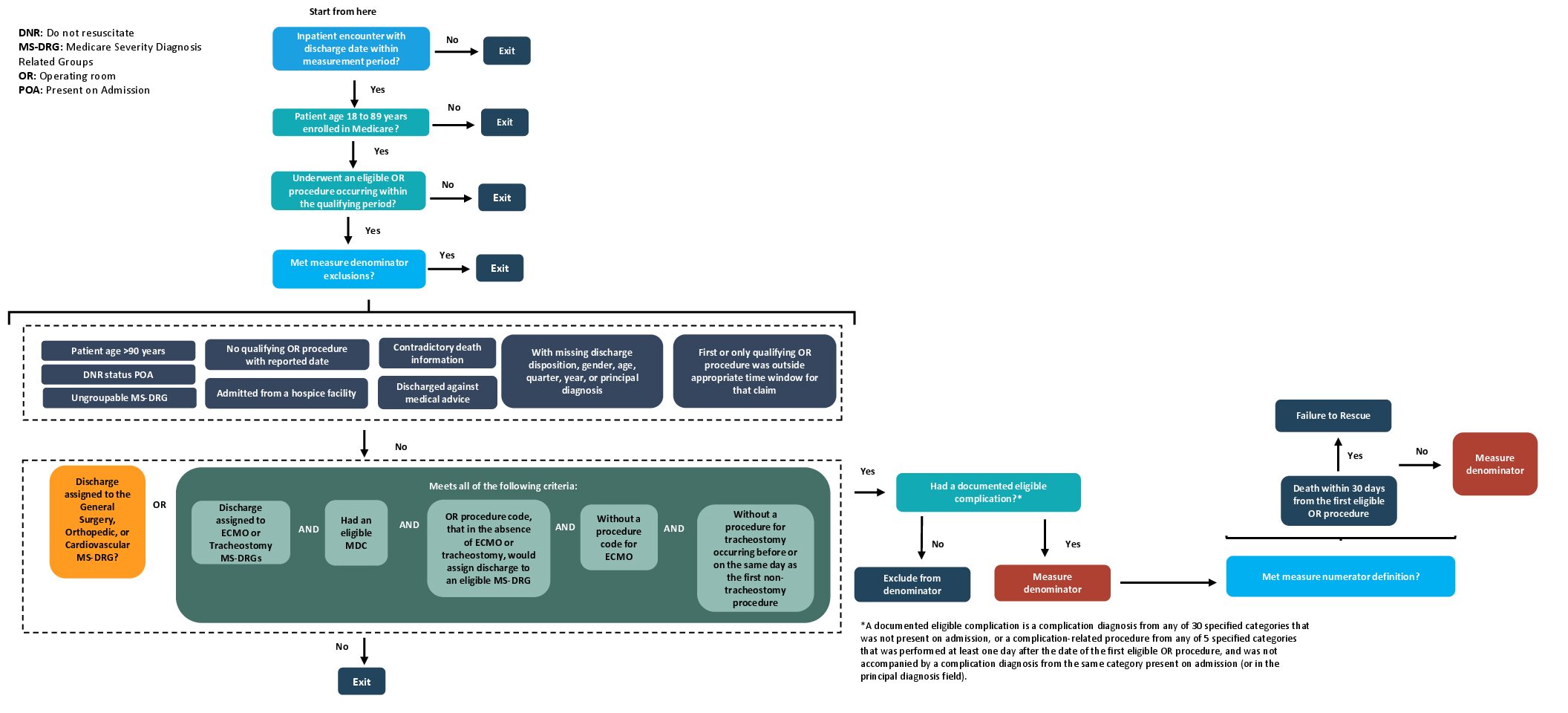
The measure is nuanced and complex. The best article I’ve read comes from the keyboard of Dr. Robert Oubre (see link below). His article includes the complications that trigger the metrics as well as a list of factors that will exclude a patient (a few include over 90 years of age, DNR status/ICD-10-CM Code Z66 POA, admitted from hospice).
Dr. Oubre also included a very handy visual from the Partnership for Quality Measurement website that I’ve included here and linked to below.
***
This is also a good time to think about query compliance as it relates to quality measures.
The new ACDIS/AHIMA physician query practice brief acknowledges the increasing pressure to improve quality measures, which as noted impact hospitals’ indirect revenue. But this pressure can result in ethical violation. The brief spells out an example of a quality specialist requesting record alternation. Per ACDIS/AHIMA:
A patient experiences hemorrhaging following a procedure. A quality specialist contacts the attending physician and requests that the documentation be modified to attribute the hemorrhage to a pre-existing condition rather than the procedure, thereby avoiding a Patient Safety Indicator (PSI).
Violation: This request directs the provider to a predetermined conclusion and incentivizes documentation that may not accurately represent the clinical picture. If there is genuine clinical ambiguity about the etiology of the hemorrhage, the appropriate pathway is a compliant query that presents clinical indicators and allows the provider to exercise independent judgment.
Were the hemorrhaging to result in patient death, that directive could move them inappropriately out of the FTR measure.
References
- Oubre’s Digest, Failure to Rescue: Understanding the measure that replaced PSI-4: https://droubredigest.beehiiv.com/p/failure-to-rescue
- Norwood, New CMS claims-based surgical quality measure is in effect; are you ready?: https://www.norwood.com/new-cms-claims-based-surgical-quality-measure-is-in-effect-are-you-ready/
- FTR flow graphic: https://p4qm.org/sites/default/files/2023-11/FTR%20measure%20flow.pdf
Related News & Insights
If a GLP-1 drops your BMI under 35, is morbid obesity off the table?
By Brian Murphy At the ACDIS conference last week, an interesting obesity coding question posed during a…
Medical Record Maestro: Reimagining CDI in the Age of AI and the Longitudinal Record
Download the episode here. We need a “human in the loop” in mid-revenue cycle work, experts say. What they fail to address is the…


