By Jason Jobes, SVP Solutions
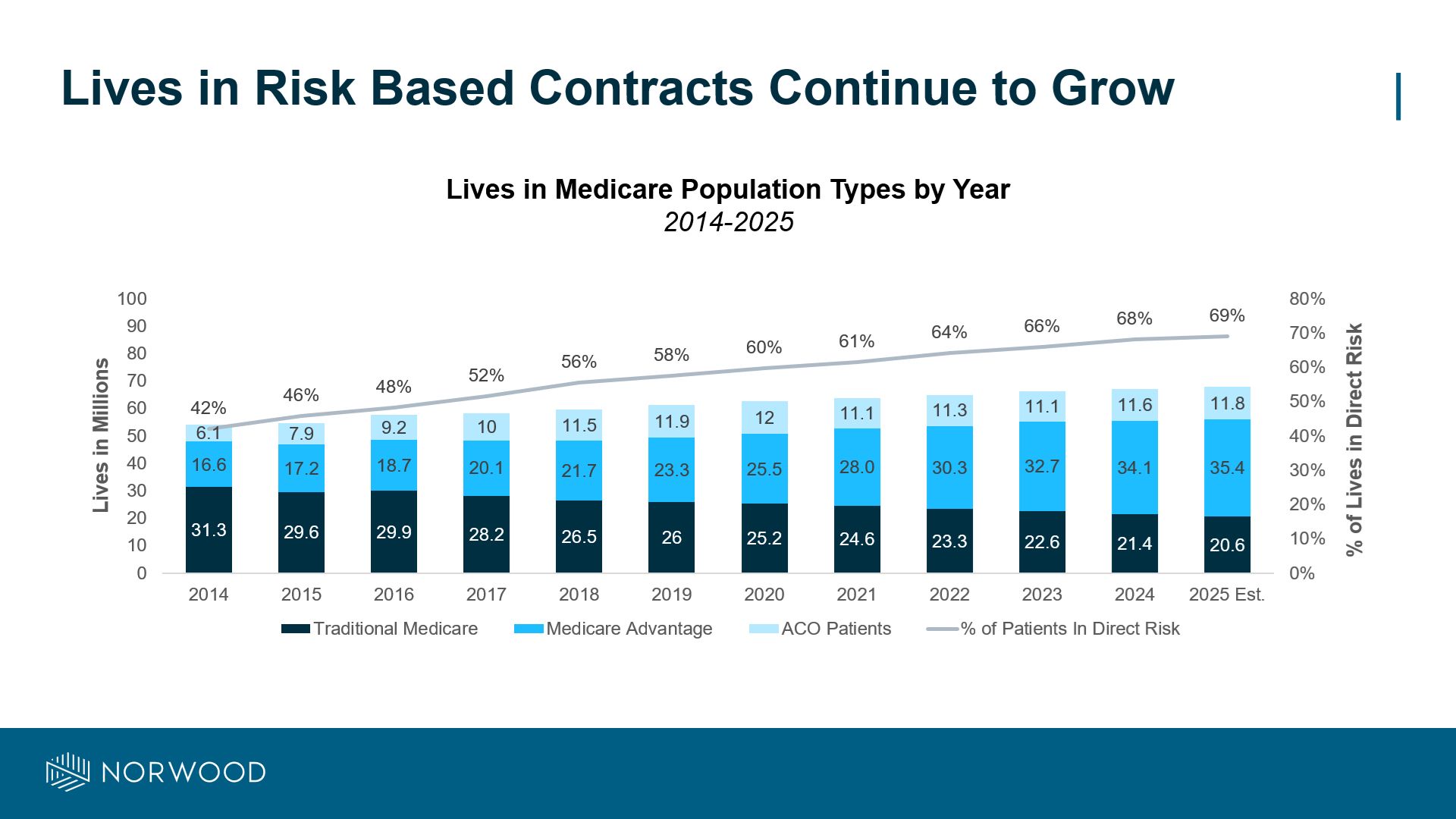
Nearly 70% of all Medicare lives are now in contracts that directly tie payment to patient complexity — a number that has surged from 42% in just a decade. As this shift accelerates, organizations must recognize that risk adjustment accuracy isn’t optional — it’s mission-critical.
To succeed, leaders need to understand these three key concepts and focus on them:
- Attribution Defines Success
In value-based care, network management is everything. To get credit for the patients you serve, you need a strategy that: Ensures patients are seen regularly; attribution with health plans is accurate, and; patients are actively engaged within your delivery system.Given access constraints across the country, organizations must build operational processes to assess attribution and maximize participation in risk contracts. - The Shift Toward Value-Based Care
Medicare Advantage and ACO enrollment have steadily outpaced traditional Medicare. Today, nearly 7 in 10 Medicare patients are in risk contracts where payments depend on risk scores that reflect patient acuity. Outpatient CDI programs are no longer “nice-to-have” — they’re essential to ensure risk scores accurately capture the complexity of your patient population. - Audits Will Define Winners and Losers
CMS continues to expand oversight, most recently through RADV mandates for MA plans. Similar measures for ACOs are likely on the horizon. A robust audit strategy is critical to identify documentation gaps and protect revenue integrity. Those who prepare now will be best positioned to withstand increased regulatory scrutiny.
Bottom Line:
Organizations that get attribution right, align with the shift to value, and build audit-ready infrastructure will not only protect revenue — they’ll be positioned to thrive in the future of Medicare risk adjustment.
If you need help, we’re here
As a reminder, this is what we do at Norwood. If you are in a risk-based contract and need help with revenue optimization or protection, contact me anytime at jason@norwood.com.
Related News & Insights
Don’t sleep on two important new changes hitting Jan. 1: Mandatory TEAM model and CMS-HCC V28 full payment shift
By Brian Murphy January 1 is rapidly closing in, and 2026 is bringing new rules and…
2026 OPPS final rule does no favors for our nation’s hospitals
By Brian Murphy The OPPS final rule, incredibly late this year, is finally out. Here I piece…



